
27. Feb 2026Business, Insight
The Digital Experience in Insurance: From Passive Contracts to a Useful Tool
Insurance companies are moving beyond viewing mobile interfaces merely as repositories for policies and are transforming them into smart platforms that manage health, property, and finances in real time. This analysis, based on the market expertise of the GoodRequest agency, combines a business perspective with the real-world needs of digital service users.


💡 What you will find in this report:
- InsurTech trends: Why ecosystems are winning and how AI is transforming claims processing efficiency. Find out where to invest so you don’t fall behind the market.
- Barriers and challenges:Identifying critical pain points that drive users to competitors and unnecessarily burden customer support.
- Segment Profiling: A detailed look at the expectations of different generations, from digital natives to seniors who are gradually adapting.
- Strategic Checklist 2026: Concrete steps for CEOs and product leaders on how to translate the digital experience into real revenue growth.
🚀 1. Key Trends: How Technology Is Defining the New Digital Experience
Digital transformation isn’t just about converting paper documents into digital formats. Its goal is to create services that make the insurance company a useful partner in everyday life.
Trend A: All-in-One Ecosystem (More Than Just Insurance)
The app is becoming the digital hub of life, where clients can manage both their health and assets in one place. Abroad, it is common to expand this space to include value-added services.
- Demand for solutions: Up to 73% of policyholders express interest in packages combining insurance with wellness services and counseling.
- Financial integration: Integrated payments are key to success. Users want to manage their accounts and purchases within their digital experience without leaving the platform.
Trend B: AI as a driver of efficiency and personalization
Global investment in AI-powered technologies grew by 40% in Q2 2024. Artificial intelligence is evolving from a futuristic concept into a tool that significantly accelerates processes.
- Lightning-fast claims processing: Thanks to GenAI, Lemonade has accelerated claims processing by 25%.
- 24/7 availability: In one case, the deployment of 24/7 AI chatbots increased interest in purchasing insurance by 11% thanks to immediate responses.
Trend C: Prevention and Rewarding Responsibility
The future of insurance is moving toward promoting health and preventing losses.
- Economic benefits: A focus on prevention could save nearly €595 billion in healthcare costs in Europe by 2040.
- The importance of gamification: Oscar Health found that 87% of users who actively tracked their steps in the app also used online counseling much more frequently.
🚧 2. Obstacles: What hinders a seamless digital experience?
Even the most advanced technology won’t help if users encounter barriers that frustrate them and drive them to visit a branch in person.
- Lack of transparency: If a user cannot see the status of a claim after reporting it (Received → Under Review → Approved), they unnecessarily burden customer support.
- Complex login: Requiring a contract number is a major point of user frustration in reviews. The future belongs to biometrics and PIN codes.
- Service fragmentation: Users expect the same tools on mobile and on the web. Differences in functionality create a negative experience.
- Unclear benefits: If benefits are hard to find or have "hidden catches," customers lose loyalty.
👥 3. User Profiles: Expectations and Business Value of Segments
A high-quality digital experience requires an understanding of each group’s lifestyle and financial background.
Gen Z and Millennials (18 – 34 years old): The Digital Generations
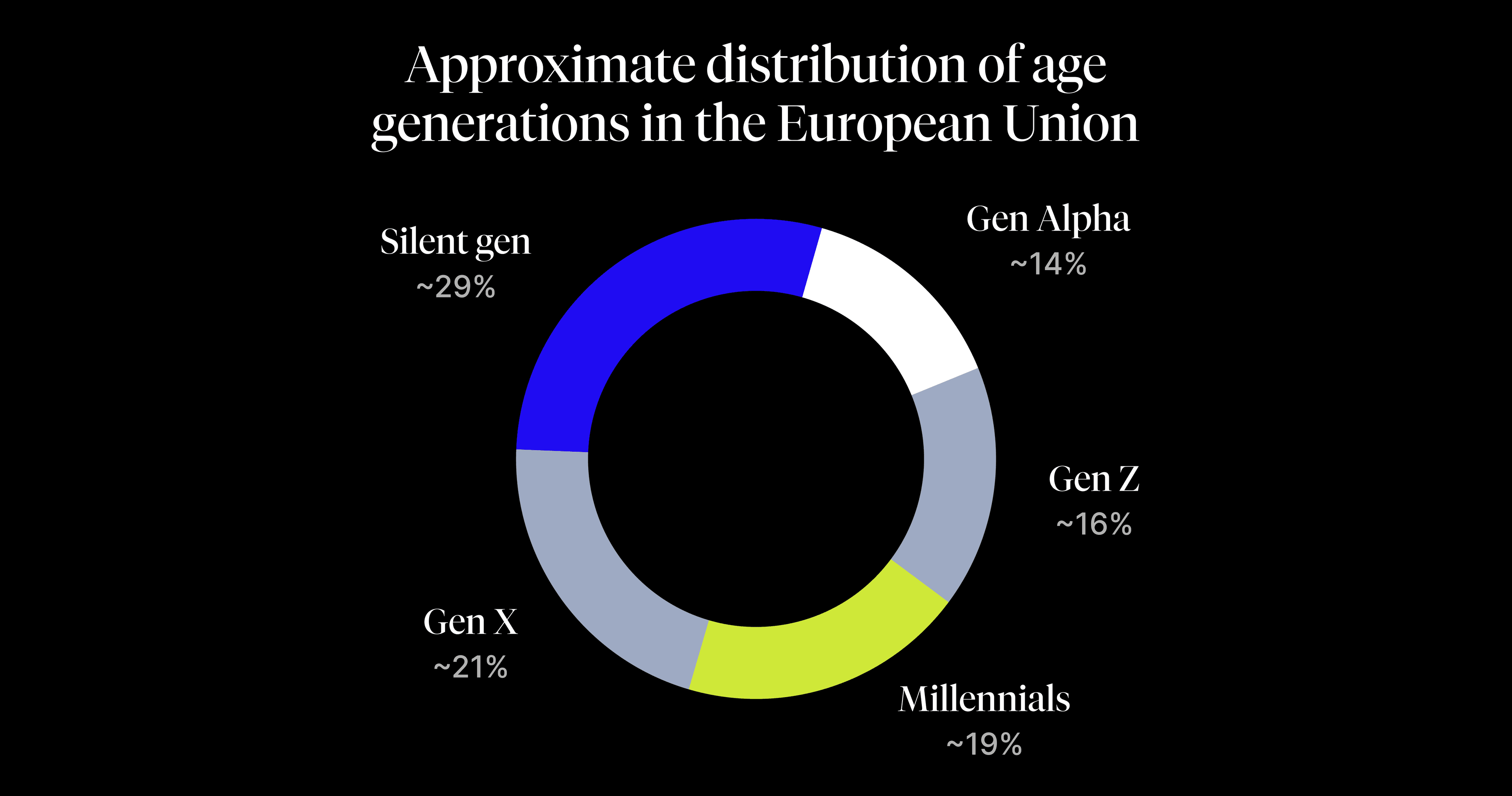
- Approximate market share: Approximately 35% of the EU population (Gen Z 16% + Millennials 19%).
- Policyholder profile: They are building their careers and establishing themselves; they typically prefer short-term rentals, travel, and own tech devices. They have high potential for travel and gadget insurance.
- Digital behavior and expectations: The smartphone is their primary tool, and they demand real-time interaction. Biometrics is a mandatory standard; purchasing and managing insurance must be a simple process requiring just a few clicks directly on a mobile device.
If Face ID is the new standard for young people, why are we still forcing them to remember passwords? Passkeys show what logging into apps will look like without them.

Young families (ages 25 – 45)
- Approximate market share:19%.
- Profile and business value: The most active segment in terms of life changes. They own real estate (mortgages) and cars, and invest in their children’s safety and health (Gen Alpha – 15% share). They are a key segment for life and property insurance.
- Digital behavior and expectations: Time is their most precious asset; technology is a natural part of their identity. They require the ability to manage family finances and health records in one place.
Gen X and Older Millennials (35–54 years old)
- Approximate market share: Approximately 21% of the EU population (Gen X).
- Policyholder profile: The most creditworthy segment with stable income. They own homes, vacation homes, and often multiple vehicles. They represent the highest “Customer Lifetime Value.”
- Digital behavior and expectations: They view technology pragmatically as a time-saving tool. Key priorities for them include online tracking of application status and transparency throughout the entire process without unnecessary bureaucracy.
Seniors / Baby Boomers (65+)
- Approximate market share: Approximately 29% of the EU population (Silent Generation / Boomers).
- Policyholder profile: They have established themselves, own real estate, and are primarily concerned with property insurance and life/health coverage.
- Digital behavior and expectations: Their digital literacy is constantly growing, but they require maximum clarity and clear benefits. Their priorities include easy access to e-prescriptions, an overview of copayments for medications, and large, legible fonts.
✅ 4. Checklist for 2026: Strategic Priorities
Companies considered technology leaders achieve up to 37% higher revenue. For 2026, we identify the following six pillars as key technological challenges:
- Biometric access: Logging in without having to remember complex credentials.
- End-to-end mobile claims processing: A complete process from reporting a claim with a photo to receiving payment directly in the app.
- Hyper-personalization: Content and offers tailored to the user’s current situation (family, health).
- 24/7 digital assistance: Support that guides users 24/7 when selecting insurance or explaining terms.
- Seamless purchase: A maximally simplified sales process with auto-fill data
- Smart notifications: Alerts about insurance expiration or outstanding payments that genuinely help the client.
💡 Prevention tip: Motivate users to be responsible before damage occurs. Reward them for safe drivingor regular preventive health care.
🏁 Conclusion: A Balanced Path to Success
Between 2026 and 2030, we expect pressure to grow in the insurance market to provide the best possible digital experience. Simplicity, functionality, self-service, and assistance will become the standard. An advanced experience includes the integration of AI into everyday use, a rewards system for loyal customers, and gamification.
However, it is essential to remember that an app is not a product, but a channel. Even the best digital experience cannot compensate for a subpar core service – such as an unfavorable offer, slow claims processing, or misleading communication. Insurance companies must not view the app merely as a "quick win", but as a tool for building long-term relationships and customer loyalty. Those who fail to offer attractive insurance and remain stuck in low levels of digitization and complex processes will be left behind.

Related articles

Are you facing a problem, or is it just FOMO that you are missing out on the AI trend?


Why don’t your users finish registration?


Trends in banking apps that drive customer retention
